How is herpes zoster migrans neuralgia treated?
How is herpes zoster migrans neuralgia treated?
Clinical definition of postherpetic neuralgia
Most foreign studies define postherpetic neuralgia as nerve pain that remains after the appearance of the rash (90-120) days, but in our clinical work when the patient's pain is more than one month, we tend to treat it according to the principles of postherpetic neuralgia management, because the disease often causes serious impact on the patient's life, and it is desirable to give early intervention to improve the patient's quality of life.
Prevention of postherpetic neuralgia
1. Early and adequate use of antiviral drugs:Antiviral therapy has a positive effect on the prevention of postherpetic neuralgia. Early use of antiviral drugs can effectively reduce viral load and toxicity, inhibit viral replication before the virus causes further nerve damage, and thus reduce the chance of postherpetic neuralgia. It has been reported that the use of antiviral drugs within 72 hours of the onset of herpes zoster can significantly reduce the incidence of postherpetic neuralgia, and that the duration of treatment should be as long as possible, up to 2 weeks, or as long as appropriate.
2. Shingles vaccination:Currently, the more internationally recognized method of preventing herpes zoster and postherpetic neuralgia is shingles vaccination. Live herpes zoster vaccine can reduce the incidence of herpes zoster by 50% and reduce the incidence of postherpetic neuralgia by 2/3. However, it should be used with caution in immunocompromised individuals and is ineffective in patients on antiviral medications.
3. Combined physiotherapy:Clinical studies have shown that a broad band of ultraviolet B spectrum (UVB) light may be beneficial in the prevention and treatment of postherpetic neuralgia due to its excellent anti-inflammatory properties and also reduces nerve damage. Other studies have indicated that transcutaneous electrical nerve stimulation for the treatment of herpes zoster is comparable to antiviral medication and is better at reducing and preventing postherpetic neuralgia.
Treatment of postherpetic neuralgia
Studies have shown that antiviral therapy in the early stages of herpes zoster can help prevent and treat postherpetic neuralgia, but it does not prevent the onset of pain in all patients. There is no specific drug treatment for patients with postherpetic neuralgia, and a single drug treatment can only relieve some of the pain, and some studies have shown that when the pain is relieved by about 50%, about 30% to 50% of the patients have adverse drug reactions. Foreign evidence-based guidelines for the treatment of postherpetic neuralgia recommend:
First-line treatment:TCAs, tricyclic antidepressants, antiepileptics, and topical lidocaine;
Second-line treatment:Opioids;
Third-line treatment:Topical administration of capsaicin.
Meanwhile, related studies have shown that despite the combination of tricyclic antidepressants TCAs and analgesics (including opioids) and topical medications (including lidocaine or capsaicin) in more than 50% of patients with postherpetic neuralgia, fewer than half of the patients achieved a satisfactory outcome, and this multi-option combination has been limited by an increase in its side effects. Related studies have shown that glucocorticoids do not reduce the incidence of postherpetic neuralgia. Some reports have foundCombined use of physical therapy (including moxibustion, fire cupping, physical therapy) supplemented by medication is superior to medication alone.The main reason for this is that physiotherapy can improve the blood supply to the damaged ganglia, which helps its nutritional access and speeds up recovery.
Feel free to like plus follow and participate in the discussion haha!
bibliography
[1] Bu XJ,Liu TY. Current status of research on postherpetic neuralgia. Dermatology and Venereology,2018,40(2):189-192.
[2] Li TT, Wang YL, Zhao YX. Research progress on risk factors and prevention of postherpetic neuralgia. Chinese Journal of Integrative Dermatology and Venereology,2017,16(3):279-282.
Chickenpox and shingles are both infections caused by the varicella-zoster virus (another member of the herpes virus family). Shingles is a reactivation of the virus that usually occurs years later. During chickenpox infection the virus spreads into the bloodstream and infects many nerve cells (ganglia) within the spinal cord and brain nerves, where it subsequently lurks. The virus may no longer cause symptoms, or it may be reactivated years later. When the virus is reactivated, it returns to the skin from the ganglia, causing viral herpes similar to chickenpox. Herpes arranges itself on the skin by traveling along the infected nerve fibers and appears on only one side of the body.
Unlike recurrent herpes simplex virus infections, shingles usually occurs only once in a person's lifetime. However, people with a compromised immune system may have multiple episodes and may develop unusual herpes and ulcers that can appear in multiple skin areas and on both sides of the torso.
The term "herpes zoster migrans neuralgia" is incorrect. The nerve pain is felt by the patient because of chronic pain in the area of the skin that is innervated by the infected nerve, also known as postherpetic neuralgia. The exact cause of the pain is unknown. However, this does not indicate that the virus is actively replicating on an ongoing basis.
Postherpetic neuralgia can be persistent or intermittent, worsening at night or due to cold/hot stimuli, and sometimes unbearable.
Postherpetic neuralgia tends to occur in the elderly, with approximately 25% to 50% of patients over 50 years of age having some degree of postherpetic neuralgia; however, postherpetic neuralgia occurs in only 10% of all patients and almost no severe pain occurs.
In most cases, the pain disappears within 1 to 3 months, but in about 10 to 20% of patients the pain can last for more than 1 year, and even more rarely for more than 10 years.
Mild pain does not require special treatment other than non-prescribed pain-relieving medications (e.g., acetaminophen) or ointments (e.g., capsaicin). Although a large number of treatments have been attempted for postherpetic neuralgia, none have been successful in managing it routinely. Physicians also use certain antispasmodics (e.g., gabapentin and pregabalin), certain antidepressants (e.g., amitriptyline), and topical lidocaine ointment. Opioids are sometimes required. Direct injection of cortisol into the cerebrospinal fluid is rarely used, but may be helpful.
Involvement of the facial nerve, which innervates the eye, can be very serious and may affect vision if not treated properly. The facial nerve innervating the ear can also be involved, sometimes causing pain, localized facial paralysis, and loss of hearing.
Those who suspect shingles should seek immediate medical attention; early treatment can be effective. The physician asks the patient to precisely describe the location of the pain. The presence of pain in a more vague band of area on one side of the torso suggests herpes zoster. If there are characteristic blisters (appearing on the skin in one dermatome), the diagnosis is clear.
Treatment should be started as early as possible, preferably in the early stages of the disease; treatment given 72 hours after the appearance of the skin lesion (herpes) may not be effective. Famciclovir 500 mg 3 times daily for 7 days or valacyclovir 1 g 3 times daily for 7 days have better bioavailability than oral acyclovir 800 mg 5 times daily for 7-10 days and are therefore preferred as a treatment for herpes zoster. Corticosteroids accelerate recovery and reduce pain accordingly, but do not reduce the incidence of postherpetic neuralgia.
Postherpetic neuralgia is difficult to treat although gabapentin, capsaicin ointment, and lidocaine cream can be used. Therefore the use of pain medications and intrathecal injections of methylprednisolone may be necessary and beneficial.
Medication should be started as soon as the disease is suspected, if possible before the blisters appear. Medications used three days after the blisters appear may not be effective. These medications do not cure the disease, but help relieve symptoms and shorten the duration of the disease. Some practitioners use a combination of Western and Chinese medicine to treat the disease, which is more effective, such as Rejuvenate Liquid to apply to the herpes area and Green Peng Ointment to apply externally to the lesions. If the viral infection encroaches on the eyes and ears, a specialist should be consulted.
Wet gauze compresses can reduce pain, and pain-relieving medications are usually necessary. Nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen may be tried, and oral narcotic analgesics are often used (must be diagnosed and prescribed by a treating physician or a physician who specializes in pain). To prevent bacterial infection, people with shingles should keep their infected skin clean and dry, and should avoid scratching the blisters.
Focus on prevention!
In keeping with the leading spirit of the DCHW App, we emphasize prevention! For children and susceptible adults, the varicella vaccine can be administered to prevent the first infection. the shingles vaccine can be used to strengthen the immune response to reduce the incidence of herpes zoster in the elderly population over the age of 60, regardless of whether or not they have ever had chickenpox.
Herpes zoster, also known as "spider sores, snake string sores, wrapped waist dragon, snake coiled waist" and so on, just listen to the name feel very powerful? By the way, it is a common skin disease caused by chickenpox-herpes zoster virus, which is prevalent in middle-aged and elderly people, and the incidence rate increases significantly with age. Haha, although this disease is self-limiting, rarely life-threatening, after healing can get a longer immunity, generally rarely reoccur. However, the most powerful trick is not the blisters that look a bit scary, but the complication of posterior neuralgia. It can cause people to be in so much pain that they can't eat, sleep or play, and some people have even tried to kill themselves, scary, right? There's no need to rush, here's what a professional pharmacist has to say about how to treat it with medication and keep it under control.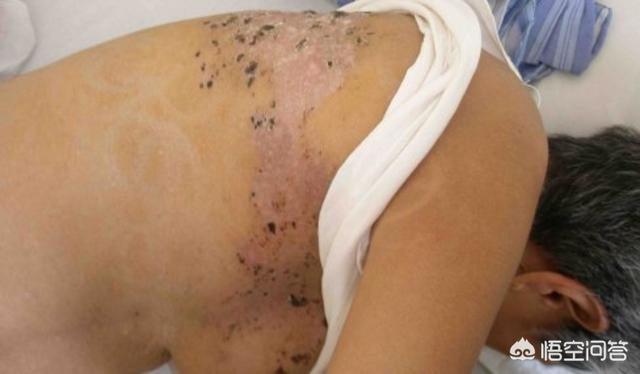 Postherpetic neuralgia (PHN)It is a common late complication of herpes zoster, which occurs in elderly and immunocompromised patients, and is clinically characterized by intractable persistent vague pain with paroxysmal severe pain.The incidence of PHN is 19.2% of the herpes zoster-affected population, and increases with age. The average age of onset of herpes zoster is 67 years, and the incidence in patients over 50 years of age is approximately 14 times higher than in patients under 50 years of age.It commonly occurs unilaterally in the chest, lower back, trigeminal nerve, or neck. The area of pain is usually wider than the area of herpes and rarely occurs bilaterally. The pain can be burning, cutting, electric shock, pinprick or tearing.
Postherpetic neuralgia (PHN)It is a common late complication of herpes zoster, which occurs in elderly and immunocompromised patients, and is clinically characterized by intractable persistent vague pain with paroxysmal severe pain.The incidence of PHN is 19.2% of the herpes zoster-affected population, and increases with age. The average age of onset of herpes zoster is 67 years, and the incidence in patients over 50 years of age is approximately 14 times higher than in patients under 50 years of age.It commonly occurs unilaterally in the chest, lower back, trigeminal nerve, or neck. The area of pain is usually wider than the area of herpes and rarely occurs bilaterally. The pain can be burning, cutting, electric shock, pinprick or tearing.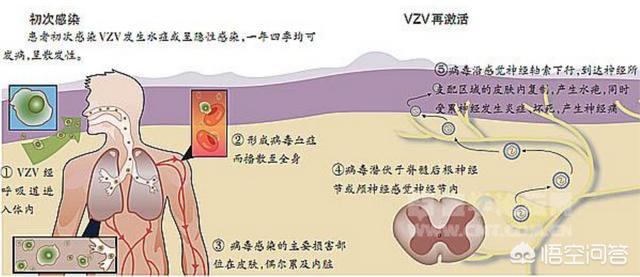
First-line medications for PHN include calcium channel modulators (pregabalin and gabapentin), tricyclic antidepressants (amitriptyline), and 5% lidocaine patches or capsaicin patches
Second-line drugs include opioids and tramadol.
Other pharmacologic treatments include inflammatory skin extracts from cowpox-vaccinated rabbits, topical capsaicin, other antiepileptic drugs (lamotrigine, valproate, topiramate), and meprobamate.
NSAIDs are of limited use in the treatment of PHN, whereas ibuprofen is ineffective.
The answer to the above was provided by the PSM Drug Shield Public Interest Editorial Pharmacist!
The herpes zoster virus is neurophilic, it lurks in the ganglia of the posterior roots of the spinal cord, and when the body's immune function is low, the virus is triggered and moves along the nerve fibers and then to the skin where herpes occurs and the nerves become inflamed and necrotic.
In general, the older you get, the less reparative you become, and the more severe and prolonged the nerve pain becomes.
Although shingles is a self-limiting disease, the sooner you get regular treatment, the less likely you are to have an episode of postherpetic neuralgia.
Persistent pain for more than 1 month after clinical cure of herpes zoster can be called postherpetic neuralgia, which is characterized by the following features:
1. There is obvious distribution of pain and tactile abnormalities according to the innervated area;
2, the nature of the pain has a cutting pain, pinprick pain, radiating pain, burning pain and so on;
3. Accompanied by symptoms other than pain: such as itching, ants sensation, twitching;
4. Severe pain makes the patient's psychological burden heavy, depression and suicidal tendency.
How to treat postherpetic neuralgia:
1, Western medicine conventional treatment has internal drugs such as pregabalin, carbamazepine, gabapentin, antidepressants, etc.; externally applied ointment has capsaicin ointment, lidocaine cream; minimally invasive interventional therapy includes nerve block, nerve destruction, pulsed radiofrequency therapy and so on.
2. I generally apply Chinese medicine treatment in clinical practice, which includes internal Chinese medicine and external Chinese medicine treatment:
Herbal internal medicine I generally use in the treatment of postherpetic neuralgia in middle-aged and older people. Why do young people with shingles seldom have neuralgia? Because they have stronger immune function and better repair ability. The middle-aged and elderly people have poorer immune function, poor blood circulation, poor repair function, so it is easy to leave behind neuralgia, in the Chinese medicine identification of Yang deficiency type of constitution accounted for the majority of these patients.
What is a Yang deficiency type of constitution? Symptoms include fatigue, lethargy, fear of cold, not wanting to move, daytime sleepiness, sleeplessness at night, stomach fear of cold, wanting to eat hot food, etc. This type of constitution belongs to the yin constitution in traditional Chinese medicine, and commonly used remedies include Ephedra, Epimedium, and Fungus with Hoshi, Si-Yi Tang, Cinnamon Branches Going to Shao-Yang plus Ephedra, Epimedium and Fungus with Hoshi, Gui Zhi plus Epimedium Tang, etc., which are used to dissipate cold and eliminate stasis and to invigorate blood circulation to relieve pain by warming up the yang.
External TCM treatments include fire needling, plum blossom needling, electro-acupuncture, moxibustion, acupoint injections, pricking and cupping, wrist and ankle needling, etc. Usually I choose one or two methods to go along with the treatment.
I'm Dr. Mengxue Chen from the Department of Dermatology. If you have any questions, please feel free to leave a comment under the article, and I will reply to all of them.
Click on the top right corner to follow my headline and make friends with your doctor and get useful skin science!
For this disease, according to the initial period, the late stage (refers to the sequelae of Western medical treatment in the early stage) and folk remedies to introduce a few treatment methods, I hope to be useful to patients.
Forwarding Gansu Dr. Bearden's headline dedication formula:
Post-herpetic formula: 40 grams of whole worm, 40 grams of Chaihu, 20 grams of red and white peony, 35 grams of Gui Zhi, 35 grams of Wei Ling Xian (washed), 25 grams of Xin Xin, totaling fine noodles (16 grams of dregs), 8 grams each time, 3 times a day. The medicine improved in 2 days, the pain stopped in 7 days, and the medicine was stopped.
Herpes zoster initial outbreak, can pay attention to consult Gansu famous Chinese medicine Liu Weizhong, (former Gansu health department director) which has sent online purchase artificial musk mixed with honey to cure herpes zoster party.
I remember when someone in our rural areas, take the dry tobacco pipe tobacco oil outside the herpes first around a circle, herpes that is circled, no longer grow out of the circle. Secondly, use the tobacco oil to apply on the herpes, a few days can be cured.



Herpes zoster is the folklore of the wrapped dragon, is a viral infection of the skin disease caused by viral damage to the nerves with blisters and nerve pain as the main manifestation. It is common in the elderly and lasts from three to four weeks.
Timely oral antiviral drugs within 48 hours of the onset of the disease, as well as nutritional nerve, symptomatic treatment of pain and other comprehensive treatment can shorten the course of the disease and reduce the sequelae, including neuralgia. However, some people, especially the elderly, in the early stage of the disease, the larger the scope of herpes, the more obvious the pain, the probability of postherpetic neuralgia is greater. It is generally recognized that after the blisters of shingles subside, if the pain lasts more than four weeks it is postherpetic neuralgia.
Herpes zoster neuralgia about 1/3 to 1/2 of the people have pain for more than a year, individual pain up to ten years, or even more, and this pain seriously affects the patient's psychological state, and serious suicidal tendencies may occur, so it deserves your attention.
There is a treatment guideline for postherpetic neuralgia treatment, and his first line of medications, the first priority, is pregabalin or gabapentin, lidocaine patches and tricyclic antidepressants. Second-line drugs include tramadol and opioids, and if the pain is obvious, minimally invasive intervention can be added to the treatment of drugs. Domestic scholars study ozone therapy also has some therapeutic effect.
Psychotherapy also plays a good supporting role. Dermatologists are no longer particularly good at postherpetic neuralgia treatment, and the department that needs to be consulted is pain medicine.
Thank you.
Postherpetic neuralgia (PHN) treatment aims to control pain as early as possible and effectively, relieve the accompanying sleep and emotional disorders, and improve the quality of life. The principles of treatment are early, adequate amount, adequate course and combined treatment, and the main treatment methods for PHN include drug therapy and minimally invasive interventional therapy. Pharmacotherapy is the basis of PHN treatment, and the selection of therapeutic drugs should be individualized, taking into account a variety of factors, such as drug efficacy, adverse effects, drug interactions, risk of drug abuse, patient's condition and pharmacoeconomic factors. Drugs for treating PHN mainly include: ① Calcium channel modulators: starting dose of gabapentin is 300㎎ per day, and the commonly used effective dose is 900-3600㎎ per day, which needs to be slowly titrated to the effective dose over several weeks. Pregabalin is dosed at 150-600 p.p.m. daily and requires 5-7 days of gradual titration. The main adverse effects of this drug class are dizziness and drowsiness. Use should follow the principles of nighttime initiation, gradual dosing, and slow tapering. ② Tricyclic antidepressants: the most commonly used is amitriptyline, the first dose should be taken at bedtime, 12.5-25mg each time, according to the patient's response can gradually increase the dose. ③ Topical drugs: Lidocaine patch, capsaicin skin patch and so on. ④ Tramadol: the starting dose is 50-100 mg per day, and the maximum daily dose is not more than 400 mg. ⑤ Opioid analgesics: they are second-line therapeutic drugs, such as morphine, oxycodone and fentanyl. They should be used in small doses, and their efficacy and safety should be evaluated regularly; once the treatment is ineffective, they should be discontinued immediately, and they should not be used for more than 8 weeks in general. Minimally invasive interventional therapy mainly includes neurointerventional techniques (nerve block, nerve destruction) and neuromodulation techniques (pulsed radiofrequency therapy, nerve electrical stimulation techniques).
bibliography
1, Chinese expert consensus on the diagnosis and treatment of postherpetic neuralgia, Chinese Journal of Pain Medicine, Vol. 22, No. 3, 2016
2, Progress of research on the treatment of postherpetic neuralgia, Chinese Journal of Pain Medicine, Vol. 22, No. 1, 2016
The authoritative interpretation of Pharmaceutical Affairs, unauthorized reproduction, plagiarism will be punished.

Herpes zoster folk commonly known as string waist dragon, wrapped waist snake, over the waist snake, fire Dan, in the neck called lockjaw snake, Chinese medicine called raw snake. The pathogen of herpes zoster is varicella zoster virus, the virus invades the human body through the upper respiratory tract or eyelid conjunctiva causing systemic infection, the initial infection in young children manifested as chickenpox, in adults can be hidden infection. The virus invades the spinal ganglion or cerebral sensory ganglion along the sensory nerves and lies latent. When the body's immune function is low, the latent virus is reactivated, replicates in large quantities, and spreads along the sensory nerve fibers to the innervated dermatomes, resulting in the occurrence of herpes zoster.
Postherpetic neuralgia (PHN) is the most common complication of herpes zoster and occurs in about 9% to 34% of patients with herpes zoster.The pain may be burning, electric shock, cutting, pins and needles, or tearing. One type of pain may predominate, or a variety of pain may coexist. The pain is often excruciating and severely affects the quality of life. The current treatment of postherpetic neuralgia mainly includes medication and minimally invasive intervention.

1. Drug treatment
First-line therapeutic drugs:
(1) Calcium channel modulators such as pregabalin and gabapentin can not only reduce pain but also improve patients' mood and sleep, but these two drugs have the adverse effects of dizziness and somnolence, and should be used according to the principle of "starting at night, gradually increasing the dosage and slowly decreasing the dosage";
(2) Tricyclic antidepressants such as amitriptyline should be taken at bedtime for the first dose, and the dose can be gradually increased according to the patient's response. Attention should be paid to their cardiotoxicity, and their use should be avoided in patients with ischemic heart disease or risk of sudden cardiac death;
(3) Sodium channel modulators such as lidocaine, commonly available in the form of lidocaine gels and patches, which have a rapid onset of action (≤4 h), with erythema or rash of the skin being the most common adverse effect.
Second-line therapeutic agents:
(1) Tramadol is a weak opioid that acts on both mu-opioid receptors and norepinephrine/5-hydroxytryptamine receptors to achieve analgesia. Adverse effects include sweating, dizziness, nausea, vomiting, loss of appetite and difficulty urinating, palpitations, dry mouth, fatigue, pruritus, and rash. The principle of starting at a low dose and slowly and gradually increasing the dosage should be followed, as well as avoiding concomitant use with 5-hydroxytryptamine medications (e.g., amitriptyline, venlafaxine, duloxetine) to avoid the risk of 5-hydroxytryptamine syndrome.
(2) Opioid analgesics
Commonly used drugs include morphine, oxycodone and fentanyl. Treatment is initiated in small doses, with periodic assessments of efficacy and safety, and should be discontinued as soon as treatment fails. The most common adverse effects are nausea and vomiting and constipation, of which constipation is a lifelong intolerance and needs to be managed.
Other drugs: In addition to the above drugs, venlafaxine, duloxetine, skin inflammation extracts from cowpox-vaccinated rabbits, topical capsaicin, and lamotrigine are also used to treat PHN.
2. Minimally invasive interventions
Minimally invasive interventions used clinically for the treatment of postherpetic neuralgia mainly include neurointerventional techniques and neuromodulation techniques. Among them, pulsed radiofrequency and nerve electrical stimulation are more common in the clinic. Pulsed radiofrequency has no destructive effect on the structure of nerve fibers, and can improve pain and quality of life; spinal cord electrical stimulation is to place electrodes into the epidural cavity, and the electric current generated by the stimulating electrodes directly affects the conduction tracts of the posterior columns of the spinal cord and dorsal horn sensory neurons as well as the sympathetic nerve centers in the lateral horns of the spinal cord, which can effectively alleviate the pain and reduce the dosage of analgesic drugs.
In conclusion, the treatment of postherpetic neuralgia should be standardized, and the principles are: early, adequate dosage, adequate course and combination therapy. Drugs combined with minimally invasive interventions can effectively relieve pain and reduce the dosage and adverse effects of drugs. The treatment of many patients may be a long-term continuous process. Drug therapy is the foundation, should use the effective dose of the recommended drugs, pain relief to avoid immediate discontinuation of drugs, but still to maintain the treatment for at least 2 weeks, do not relax carelessly.
bibliography
1. Yu Shengyuan, Wan You, Wan Qi, et al. Chinese expert consensus on the diagnosis and treatment of postherpetic neuralgia[J]. Chinese Journal of Pain Medicine, 2016, 22(3):161-167.
2. Neuropathic pain diagnosis and treatment expert group, Fan Bifa. Expert consensus on the diagnosis and treatment of neuropathic pain[J]. Chinese Journal of Pain Medicine, 2013, 19(12):705-710.
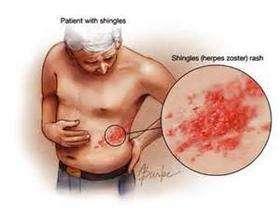 (Ear Zhao Q&A 20171225) Herpes zoster after the acute phase of the onset of the disease still some patients have pain at the site of the onset of the disease, this pain is medically known as herpes zoster postherpetic neuralgia, which can occur in all parts of the body, and in the peri-auricular area is a problem for otorhinolaryngologists to deal with. This pain is one of the more common of the many complications of herpes zoster and is a chronic complex neuropathic pain caused by persistent damage to peripheral or/and central neurons by the varicella zoster virus-stimulated immune and/or inflammatory response.
(Ear Zhao Q&A 20171225) Herpes zoster after the acute phase of the onset of the disease still some patients have pain at the site of the onset of the disease, this pain is medically known as herpes zoster postherpetic neuralgia, which can occur in all parts of the body, and in the peri-auricular area is a problem for otorhinolaryngologists to deal with. This pain is one of the more common of the many complications of herpes zoster and is a chronic complex neuropathic pain caused by persistent damage to peripheral or/and central neurons by the varicella zoster virus-stimulated immune and/or inflammatory response.
The varicella zoster virus is called chickenpox when it first strikes a child. After the symptoms of chickenpox subside, the virus lurks in the body (mostly in the nerve tissue area), and when the body's immune function is lowered, the dormant virus begins to revive, replicate, and spread along the branches of the peripheral nerves to the surface of the skin, resulting in clusters of blisters arranged in bands and significant pain, which is then called herpes zoster. Most of the pain in the area of onset subsides as the herpes subsides, but a small number of patients will remain in pain for a long period of time, which is called postherpetic neuralgia.
There is no uniform definition of the specific time of "sequelae", the domestic generally considered to be the emergence of the rash after the pain time more than four weeks, the international is the rash appeared pain lasted more than 90 days. 2015 International Academy of Pain recommended the consensus on the treatment of neuropathic pain, for the first-line drugs for postherpetic neuralgia include tricyclic antidepressants (amitriptyline, desipramine, and nortriptyline), duloxetine and venlafaxine, anticonvulsants pregabalin, gabapentin, gabapentin extended-release, and gabapentin ester, second-line medications include lidocaine pads, 8% capsaicin pads, and tramadol, and third-line medications include strong opioids and botulinum toxin. In addition to medication, there are also invasive treatments, such as therapeutic drugs or instruments that can be placed into the diseased tissue under the guidance and positioning of CT, ultrasound, and luminal scopes to achieve analgesia by blocking the nerve conduction in a less invasive way.
Neuralgia is one of the sequelae of herpes zoster. Once the attack, it will be very painful, seen a lot of patients will be in pain, seriously affecting the normal life, there are patients will not be able to endure the idea of light life.
How does this neuralgia manifest?
Neuralgia of shingles relocation is a persistent and severe pain that occurs after the healing of this disease of shingles. The skin on the diseased area will be hyperpigmented and will be red, purple or even have a reddish-brown color. There are also clinical cases where there is no scarring, but severe neuralgia still occurs.
The nerve pain that migrates from shingles is also different from normal pain. That intense and unbearable pain that comes from even the slightest touch of the skin. There are often two types of pain: a constant burning pain and a paroxysmal cutting pain. Both can occur spontaneously and when the skin is lightly touched. The pain is often relieved by firm pressure on the skin, while light touching of the skin is often intolerable. Other patients may experience intolerable itching and a sensation of ankylosis or even a dulling of sensation. Neuralgia associated with herpes zoster is usually triggered by a decrease in immunity due to overexertion, cold weather, emotional changes, and so on.
So what should be done to treat this shingles migrating neuralgia?
Postherpetic neuralgia can be treated in the pain department of your regular hospital and you can usually get good results.
There are several principles of treatment:
The first one is the treatment of nerve function regulation. Because once the nerve function is in the process of disorganization after an illness or a surgery, the response of the nervous system at this time is different from that of a normal person. Pain doctors will do some adjustments, such as using some sympathetic methods, first adjusted;
The second step is to use some nutritive nerve medications to promote nerve repair;
The third step is to control the subsidence of nerve inflammation, which requires the appropriate use of anti-inflammatory and analgesic drugs;
In the fourth step, the intervention of ozone is carried out;
The fifth step is usually accompanied by appropriate rehabilitation physical therapy to minimize the recurrence of pain.
Instructor: Wang Jiashuang, National Second Class Professor, Chief Physician, Top Ten Famous Doctors of Guangzhou. Former Vice Chairman of Pain Society of Chinese Medical Association, Chief Expert of Pain Department of Jinshazhou Hospital of Guangzhou University of Traditional Chinese Medicine, Honorary Lifetime Professor of Pain Department of Guangzhou Red Cross Hospital, Medical College of Jinan University.
Specialties: postherpetic neuralgia and cervical and lumbar disc herniation pain management.
Learn more about health science, stay tuned:Medlink Media
This question and answer are from the site users, does not represent the position of the site, such as infringement, please contact the administrator to delete.