How does diabetic ketoacidosis occur?
Diabetic ketoacidosis is the most common type of diabetes mellitus poor glycemic control of hyperglycemic emergency, common manifestations include: "three more and one less" symptoms worsening, blood glucose persistently higher than 16.7 mmol / L, blood ketones higher than normal, urine ketone positive or strong positive.
Why are people more familiar with this acute complication? Because, in addition to the calendar year physical, many sugar addicts find out they have diabetes through ketoacidosis.
The three major nutrients that supply energy to the human body include: carbohydrates (that is, glucose in the body), proteins, and fats. Under normal circumstances, the body has enough insulin, the body gives priority to the use of glucose for energy supply, so as to meet the energy needs of various organs of the body, and glucose is utilized after the direct decomposition into carbon dioxide and water and through the respiration, urine, sweat and so on out of the body.
However, when insulin is seriously insufficient in diabetic patients, glucose cannot be utilized as energy, which leads to hyperglycemia; at the same time, because of insufficient energy in the body, it needs to break down fat to produce energy. However, fat can not be completely oxidized and decomposed, thus producing ketone bodies. If a large number of ketone bodies can not be discharged from the body in a timely manner, the accumulation of ketosis in the body will cause ketosis, and ketone bodies are an acidic substance, making the blood acidic, so ketoacidosis occurs.
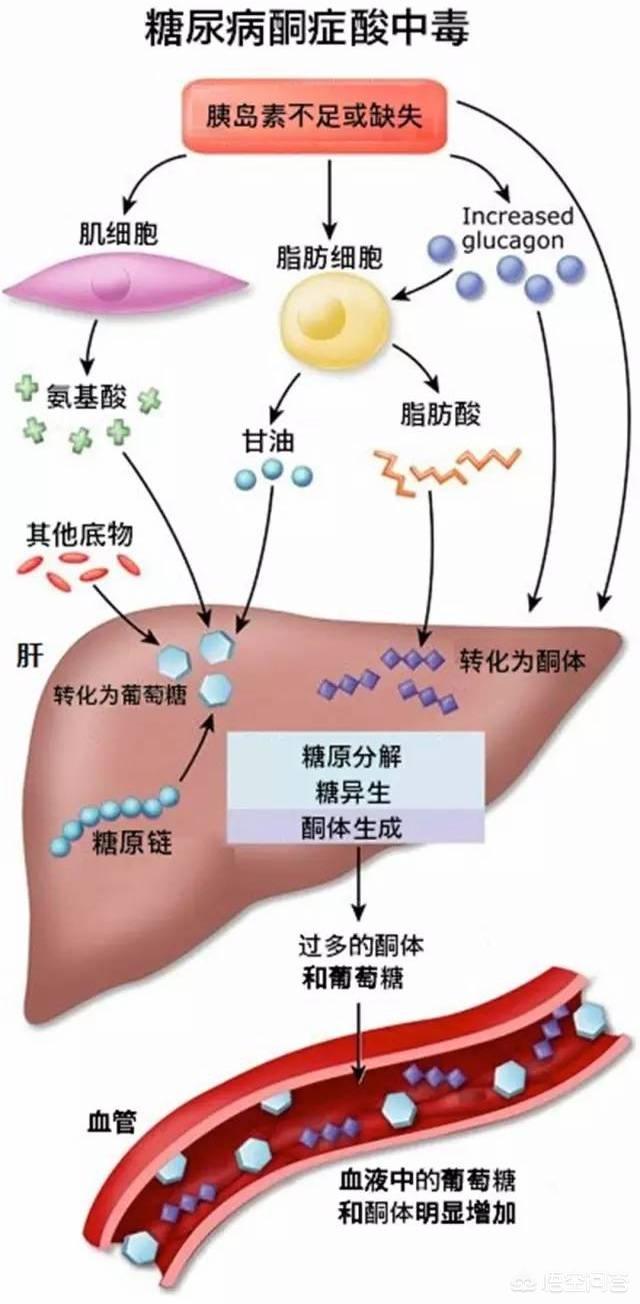
Therefore, to prevent diabetic ketoacidosis in diabetics, it is important to avoid its triggers, which most commonly include:
1, acute infection: winter and spring is good, common parts of the respiratory tract, urinary tract and skin.
2, eating disorders and gastrointestinal diseases: such as overeating, alcoholism, or vomiting and diarrhea, can aggravate the metabolic disorders of diabetes.
3. Inadequate treatment: including interruption of medication, insufficient dosage, etc.
4, other stress: including trauma, surgery, pregnancy, childbirth, mental stimulation and myocardial infarction or cerebrovascular accidents and other conditions.
diabetic ketoacidosisIt is one of the most common acute complications of diabetes mellitus, which tends to occur when blood glucose remains high, with upper respiratory tract infections being a common predisposing factor, as well as insufficient amounts of insulin, leading to insufficient insulin action and the breakdown of fats to produce ketone bodies. Ketone bodies are acidic, causing acidosis and increased urine output.
Fever can lead to a significant loss of body fluids, which leads to a decrease in blood volume, causing hypotension, which in turn leads to a state of shock. In addition, shock can lead to multiple organ dysfunctions such asAcute renal failure and acute pancreatic injury。
Under what conditions does diabetic ketosis usually occur?
Type 1 diabetes can develop in the form of ketoacidosis at first;
Discontinue or use less insulin;
Other stresses: e.g., conditions such as combined acute infection, trauma, acute myocardial infarction, stroke, etc;
Diabetic ketoacidosis can also occur in type 2 diabetes.

Clinical symptoms of various stages of diabetic ketoacidosis
Early symptoms: polyuria, dry mouth, thirst blurred vision.
Intermediate symptoms: nausea, vomiting and abdominal pain, deep and fast breathing, and an odor of "rotten apples" in the exhaled breath.
Severe symptoms: dehydration, cold extremities, coma.

What can I do to avoid diabetic ketoacidosis?
first of allMonitoring of blood glucose, fasting blood glucose is controlled at 3.9-7.2 mmol/L, postprandial blood glucose is controlled within 10 mmol/L, and if blood glucose fluctuates, immediate blood glucose is also controlled within 11 mmol/L.
Secondly.Take care to adjust the type and dose of insulinDifferent patients have different rhythms of blood glucose fluctuation and need different types of insulin at different times, so they should choose the appropriate insulin and oral medication for their situation under the guidance of their specialists.
Furthermore.Maintain a regular routineIt is vital to have a strict diet and moderate exercise to avoid infections and the occurrence of other medical conditions.
Finally, consciously learn about diabetes and manage your blood sugar scientifically. Seek medical attention as soon as ketoacidosis is suspected.

(Web image, for reference only)
Hunan Medical Chat Contributed by Shen Yanling, Emergency Department, Hunan Taihe Hospital
Diabetic patients in a short period of time blood glucose rise dramatically or type 1 diabetes patients stop using insulin, the body will appear to utilize glucose metabolic disorders, and most of the energy required for physical activities are decomposition of store to obtain, the body in order to survive, we need enough energy, so it will be compensated for the decomposition of proteins and fats to provide energy to supply the body's activities. However, the decomposition of protein and fat is not as adequate as the decomposition of glucose, will leave a lot of acidic metabolites, these things if a large number of accumulation in the body can not be effectively eliminated from the body, will exceed the limit of the body's self-adjustment induced diabetic ketoacidosis.
Typical symptoms of diabetic ketoacidosis include severe dehydration, generalized body aches, nausea, vomiting, and breathing with an unusual odor. If a diabetic patient has similar symptoms, the first thing to do is to perform a routine blood glucose and urine test, and if it is found that the blood glucose is elevated and the urine ketone body is positive, then diabetic ketoacidosis should be considered.
Diabetic ketoacidosis this disease once found, must go to the hospital for infusion treatment, on the one hand, need intravenous drip small dose insulin to drop blood sugar to improve the metabolic state of the body's energy, on the one hand, need a lot of rehydration to promote acidic metabolites excreted out of the body, at the same time at the end of the treatment, the need to adjust the long-term application of glucose-lowering program, to avoid recurrent episodes of ketoacidosis.
Find this article useful, feel free to like or recommend to friends and follow[MEDLINE MEDIA]。
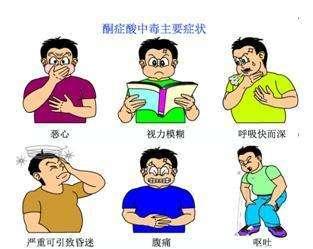
Diabetic ketoacidosis is an acute complication of diabetes mellitus, which is mainly caused by insufficient insulin in the body due to various reasons for the body to break down fat. So it mostly occurs in type 1 diabetes (absolute lack of insulin in the body) as well as type 2 diabetes with sudden discontinuation or insufficient dosage of insulin, and a variety of stressful situations: such as the combination of acute infections, trauma, surgery, acute myocardial infarction, and strokes, and so on. Because the process of the body's utilization of glucose requires the participation of insulin, but due to the lack of insulin, the body can only use lipolysis energy to supply the body with energy, and in this process, substances including acetoacetic acid, beta hydroxybutyric acid, and acetone are produced as 3 components. Known as ketone bodies, ketone bodies are produced in excess and can neither be effectively utilized nor completely excreted from the body, thus accumulating in the bloodstream in large quantities, resulting in elevated blood ketone levels. When ketone bodies are only mildly increased, the body regulates them to keep the blood pH in the normal range, which we call simple ketosis. If the ketone bodies increase further, causing the blood to become acidic and a metabolic acidosis develops, we call it diabetic ketoacidosis. After ketoacidosis, the patient's original diabetic symptoms often significantly aggravated, manifested by obvious thirst, drinking, urination, dizziness, loss of appetite, dehydration, severe skin mucous membrane dryness, poor elasticity, decreased blood pressure, deep and fast respiration, exhaled breath will have a rotten apple flavor. Further development, the patient can occur drowsiness, confusion, and even coma, if not timely rescue, can lead to death. Therefore, for diabetic patients should be actively prevented to prevent the emergence of ketoacidosis, once suspected ketoacidosis should be promptly to the hospital, so as not to delay the condition.

 Diabetic ketoacidosis (DKA) is one of the most common acute complications of diabetes mellitus, mainly occurring in type 2 diabetic patients. If diabetic patients are applying insulin hypoglycemic treatment, due to some reasons suddenly interrupt insulin injection, or without consulting a diabetes professional doctor, reduce the insulin dose at will, resulting in a short-term sharp rise in blood glucose and accelerated fat decomposition, it will be in the body of the body too much and too fast to produce a kind of acid called ketones, which accumulate in the body over the body's ability to utilize the metabolic acidosis occurs. The main manifestations are extreme thirst, dry mouth, loss of appetite, nausea and vomiting, abdominal pain, weakness of the limbs, breath smells like rotten apples, and elevated blood sugar, ketone bodies in the urine. If not treated in time, the patient may even become unconscious and comatose within a few hours, or even lose his life. It is not uncommon to see deaths due to diabetic ketoacidosis every year.
Diabetic ketoacidosis (DKA) is one of the most common acute complications of diabetes mellitus, mainly occurring in type 2 diabetic patients. If diabetic patients are applying insulin hypoglycemic treatment, due to some reasons suddenly interrupt insulin injection, or without consulting a diabetes professional doctor, reduce the insulin dose at will, resulting in a short-term sharp rise in blood glucose and accelerated fat decomposition, it will be in the body of the body too much and too fast to produce a kind of acid called ketones, which accumulate in the body over the body's ability to utilize the metabolic acidosis occurs. The main manifestations are extreme thirst, dry mouth, loss of appetite, nausea and vomiting, abdominal pain, weakness of the limbs, breath smells like rotten apples, and elevated blood sugar, ketone bodies in the urine. If not treated in time, the patient may even become unconscious and comatose within a few hours, or even lose his life. It is not uncommon to see deaths due to diabetic ketoacidosis every year.
For diabetic ketoacidosis, should go to the hospital as soon as possible, routine blood and urine tests can provide sufficient basis for diagnosis. The main factors triggering ketoacidosis are cold, fever, trauma, serious infections, severe mental shock, gestational diabetes and so on.
Diabetic ketoacidosis, the most common acute and serious complication of diabetes mellitus, as the name suggests, is associated with acidity, which is essentially an increase in the acidity of the blood, and the signs and symptoms include nausea, vomiting, polyuria, polydipsia, weight loss, and hyperventilation i.e., Kussmal respiration.
The human body has three major energy-supplying substances, generally glucose energy supply, in some special circumstances, glucose utilization disorder or glucose supply is insufficient, fat will be broken down for energy supply, fat decomposition product is ketone bodies, a large number of ketone bodies can not be excreted in a timely manner, the accumulation of ketosis in the body will cause. The ketone body is acidic, ketone body will change the blood PH value, so that the blood is acidic, ketoacidosis occurs.
Diabetic ketoacidosis does not occur for no apparent reason, it usually occurs with poor glycemic control in type 1 diabetes, and can occur in type 2 diabetes as well. The usual triggers are infections, intoxication, improper discontinuation of insulin, stroke, and other unexpected occurrences. Triggers can be present alone or multiple triggers can be present at the same time:
Inadequate treatment:This is a major trigger for patients with type 1 diabetes due to interruptions in medication, especially insulin, insufficient doses of therapeutic drugs, and the development of resistance.
Infection:This is the most important trigger of diabetic ketoacidosis. Examples include systemic infections, sepsis, pneumonia, suppurative soft tissue infections, acute infections of the gastrointestinal tract, acute pancreatitis, gallbladder cholangitis, peritonitis, pyelonephritis, and pelvic inflammatory disease.
Various stress states:It can be induced by trauma, surgery, anesthesia, pregnancy, childbirth, myocardial infarction, heart failure, and severe mental stimulation. Accelerated lipolysis secondary to diabetes mellitus with stress, or accelerated lipolysis with glucocorticoid therapy, etc.
Irregular diet and gastrointestinal disorders: Diabetic ketoacidosis is induced by over- or under-eating, eating large quantities of desserts or alcohol, or by gastrointestinal disorders that cause nausea, vomiting, or diarrhea that increase the weight of the metabolic disorders.
Sugar man health network, a temperature control of sugar platform, welcome to pay attention to the questions and answers!
[2017-12-28 Chinese Medical Science Answer]As the question is asked, thank you, to answer this question, it is necessary to understand that the complications of diabetes are categorized into acute and chronic complications, and that diabetic ketoacidosis is very common, and in some cases is even the initial manifestation of the disease, which is why it is so important to know about it.
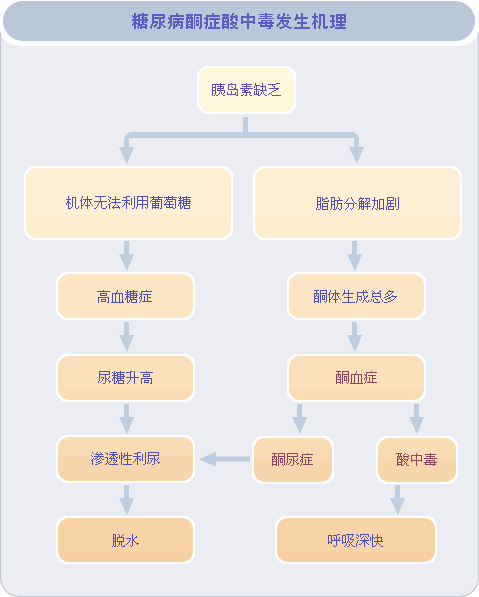
Diabetic ketoacidosis is a clinical syndrome in which the main manifestations are hyperglycemia, ketosis, metabolic acidosis and dehydration due to the severe lack of insulin activity and the inappropriate increase of glucagon, which causes the disturbance of sugar, fat and protein metabolism, resulting in the imbalance of water, electrolyte and acid-base balance. It is an acute complication of diabetes mellitus and one of the common clinical crises in internal medicine. When diabetic metabolic disorders develop to a serious stage, accelerated lipolysis, serum ketone bodies accumulate more than the normal level is called ketonemia, increased urinary ketone discharge is called ketonuria, when the clinical manifestations are collectively referred to as ketosis. Ketone bodies in the increase in the acid base, a large number of consumption of the body's reserves of alkali, and metabolic acidosis, known as DKA; such as the seriousness of the condition of the occurrence of coma is known as diabetic coma.
The occurrence of DKA is related to the type of diabetes mellitus, but not the duration of the disease, about 20% of newly diagnosed type 1 diabetes mellitus and some patients with type 2 diabetes mellitus can develop DKA. 1 diabetes mellitus has a tendency to develop DKA, and type 2 diabetes mellitus can also develop under certain triggers. In some diabetic patients, DKA may be the first manifestation of DKA. most of the clinical onset of DKA has triggering factors, and these triggers are related to increasing the body's need for insulin. Common triggers are as follows.
1. Infection: It is the most common cause of DKA. Commonly, there are acute upper respiratory tract infections, pneumonia, purulent skin infections, gastrointestinal infections, such as acute gastroenteritis, acute pancreatitis, cholecystitis, cholangitis, peritonitis and so on, as well as urinary tract infections.
2, the application of glucose-lowering drugs is not standardized: due to weight gain, hypoglycemia, poor patient compliance and other factors resulting in insulin injection of diabetic patients, sudden reduction or discontinuation of treatment; or in the case of acute concomitant diseases, did not increase the dose of insulin in a timely manner.
3. Trauma, surgery, anesthesia, acute myocardial infarction, heart failure, mental tension or severe stimulation causing stress.
4, eating disorders or gastrointestinal disorders, especially with severe vomiting, diarrhea, anorexia, high fever and other causes of severe water loss and insufficient food, if at this time insufficient insulin dosage or interruptions, reduce the dosage is more likely to occur.
5. Pregnancy and childbirth.
6, insulin resistance:Insulin insensitivity or insulin antibody production due to receptor and signaling abnormalities can lead to reduced efficacy of insulin.
7、Accompanied by excessive secretion of hormones antagonizing insulin, such as acromegaly, cortisolism, or massive application of glucocorticoids, glucagon, sympathomimetic neuroactive drugs.
8. Uncontrolled or aggravated diabetes, etc.
Hope you can help, welcome to pay attention to the "Chinese medical science platform" headlines, to get more professional and original medical science knowledge, this article for the original content, unauthorized refused to reproduce.
Diabetic ketoacidosis, loosely described as the body's酮 bodyPoisoning caused by too much of it, which causes the blood to become acidic.
What are ketone bodies?
Ketone bodies arefatIn the liver.decomposition productUnder normal circumstances, the body produces a small amount of ketone bodies, which are transported with the blood to the tissues and utilized as a source of energy; because of the small amount and low concentration, they are undetectable in the urine, so urinary ketone bodies of a healthy person should benegatives(Medical reports usually have this item).
- But if there is not enough insulin in the body and there is excessive/abnormal lipolysis (because there is a malfunction in the utilization of sugars and the body has to break down fats), then the concentration of its product, ketone bodies, climbs, at which point some of them will be eliminated through the urine, while others will continue to remain in the body, and when too much builds up, it will lead to the blood becoming acidic, and thus the development of "diabetic ketoacidosis".

At this time, the original symptoms will be significantly aggravated, such as significant polyuria, thirst, dizziness, loss of appetite; dehydration is severe people with dry skin and mucous membranes, poor elasticity, decreased blood pressure, deep and fast breathing, and breath smells like rotten apples;
Further development, the patient can occur drowsiness, confusion, or even coma, if not timely rescue will be in an extremely dangerous situation.
How is it prevented and treated?
1) Follow medical advice and regular treatment;
2) Reasonable dietary and exercise habits: a special reminder is needed that theTo treat diabetics' loss of appetite as a more serious problem, rational feeding, hydration, and medication to avoid the onset and progression of ketoacidosis;
(3) Keep rational, do not indiscriminate treatment. Mislistening to exaggerated advertisements, misuse of "bias" and terminate the regular treatment is very dangerous; life is a lot of people are mistakenly believe that a certain method can cure diabetes and stop using insulin, the result is ketoacidosis, this lesson is really painful to themselves and others ah;
Reference: Gu Jingfan, Du Shoupin, Guo Changjiang, Modern Clinical Nutrition, Second Edition. Beijing: Science Press, 2009
Wish you good health, I am Vivi, a nutritionist who wants to live 120 years, warm and reliable, welcome to follow and grateful for the trust.
Diabetic ketoacidosis (DKA) is a clinical syndrome with hyperglycemia, hyperketonemia, and metabolic acidosis caused by insulin deficiency in the body, which is an acute comorbidity of diabetes mellitus and one of the most common emergencies in internal medicine.
(i) Morbidity and mortality The incidence of DKA has not changed much in Western countries over the past 10 years, despite the general improvement in medical conditions. The incidence rate of DKA in western countries is 4.6‰, and the annual incidence rate of DKA among 1,000 diabetic patients in the United States is 3-7, of which 20%-30% are new patients with insufficient knowledge of diabetes. The mortality rate is 1% to 19%, with an average of 14%, and 21.4% reported by the Union Hospital in China. The mortality rate is higher in the older age group, and factors affecting poor prognosis include hypertension, hyperglycemia, acidosis, azotemia, and severe complications.
(ii) Predisposing factors Predisposing factors are infection in more than 50% of cases, with increased glucagon and cortisol secretion during infection, followed by thrombophilia, which is unknown in 25% of cases. Intentional discontinuation of insulin therapy is rare, but interruption of insulin infusion during treatment with continuous subcutaneous insulin infusion (CSII), in the absence of a malfunction of the insulin delivery system, is a clear cause of DKA in recent years. Eating less or incorrectly reducing insulin doses increases the risk of DKA. In recent years, blood glucose test strips have replaced urine tests, resulting in a failure to recognize ketonuria. Appropriate patient education can often prevent the occurrence of DKA triggers and reduce the incidence of DKA.
II. Diagnosis
(a) Clinical manifestations According to the development of the disease, it is divided into three stages: diabetic ketosis, diabetic ketoacidosis and diabetic ketoacidosis coma. Typical manifestations of DKA include hyperventilation in acidosis, dehydration, hypotension, warm skin and hypothermia, rapid heart rate, impaired consciousness, and in 10% of the cases, complete coma. Exhalation smells like rotten apples. Precursors are excessive thirst and urination, nausea, vomiting, anorexia, and in a few cases gastrocnemius muscle spasm and abdominal pain, which can be misdiagnosed as acute abdomen.
(ii) Laboratory tests: urine glucose and ketone bodies are strongly positive, but when renal function is severely impaired and the threshold is increased, urine glucose and ketone bodies can be reduced. Most of the blood glucose is 16.7-33.3mmol/L (300-600mg/dL), sometimes up to 55.5mmol/L (1 000mg/dL) or more. Blood ketone bodies are significantly higher than normal, CO2 binding capacity is lowered, and in severe cases, it is below 10 mmol/L. Blood pH is lowered.
The diagnosis is made on the basis of a history of diabetes, positive blood and urine sugars and ketone bodies. If there has been a prolonged period of time without food, the urine may be negative for glucose. Blood and urine ketone bodies are based on nitroprusside, which reacts only with acetoacetic acid and only slightly with acetone. Therefore, in severe acidosis, a false negative may occur if β-hydroxybutyrate is significantly greater than acetoacetate.
After diagnosis and resuscitation are initiated, further laboratory tests include blood gas analysis, blood creatinine for dehydration and prerenal failure, and BUN for protein catabolism and metabolism. The four electrolytes help to calculate the anion gap (AG) = (Na+++ K+) mmol/L - (Cl- + H2CO3) mmol/L, with a normal value of 12 ± 2 mEq/L. If this is greater than 14, it is indicative of anion gap acidosis, but it can be less than 12 in hyperchlorhydria. Hyperglycemia decreases serum sodium measurements, with a 2.78 mmol/L increase in the former and a 1 mmol/L decrease in the latter. Severe hyperlipidemia may also indicate pseudo hyponatremia. A high serum potassium value indicates an acute episode of DKA and poor urinary excretion. A low value of serum potassium indicates a significant systemic loss of potassium. Plasma osmolality is calculated using the following formula: 2(Na++K+)mmol/L + glucose mmol/L + BUN mmol/L = osmolality mmol/L, which is fairly consistent with osmolality measurements. Find the source of infection and sensitize bacterial cultures. Blood leukocytes and ketone levels do not correlate and do not change with or without infection, and mild infections often do not produce a fever. The electrocardiogram helps to visualize the heart and is used as a monitor to correct hypokalemia. The ECG changes produced by acidosis itself sometimes appear to be ischemic. A chest X-ray should be routinely performed.
III. Treatment
(In DKA, there is often severe water loss, resulting in poor perfusion of tissue microcirculation, and insulin cannot effectively enter the interstitial fluid to exert its biological effect. Fluid infusion is the first and the most critical measure when rescuing DKA. Regardless of the route of insulin application, insulin can fully play its role only when effective tissue perfusion is improved and restored.
Rehydration mainly involves the type, amount and rate of rehydration.
1. Types of infusion Firstly, isotonic solution (0.9% saline) should be infused. Since hypotonic solution (0.45% sodium chloride or 2.5% glucose) may cause cerebral edema and hemolysis, it is generally advocated that hypotonic solution should only be considered when plasma osmolality is more than 350mOsm/L and sodium is higher than 155mEq/L. When osmolality drops to 330mOsm/L, saline should be used instead. When osmolality drops to 330 mOsm/L, saline should be used instead. When blood glucose falls below 250 mg/dL (13.89 mmol/L), 5% dextrose solution or 5% dextrose saline should be used.
2. the total amount of rehydration Depending on the degree of dehydration, the first 24h of the rescue can be considered 10% of the patient's body weight in fluid weight, such as 60kg with 6,000ml. or according to the degree of light weight rehydration, such as diabetic ketoacidosis, the amount of fluid about 2,000-3,000ml; diabetic ketoacidosis, the amount of fluid about 3,000-4,000ml; diabetic ketoacidosis coma, the amount of fluid about 5,000-6,000ml. The amount of fluid needed is about 5,000-6,000ml.
3. Infusion rate: first fast and then slow, 1-2L in the first 2h, then 1L every 4-6h. For elderly patients with coronary artery disease and other cardiovascular diseases, rehydration should not be too much too fast. If necessary, use central venous pressure to assist observation. When rescuing DKA patients, it is necessary to open two venous infusion routes, one to ensure the infusion of insulin and the other to ensure rehydration.
(In recent years, a large number of basic researches and clinical practices have shown that small-dose insulin treatment program has the advantages of simplicity, effectiveness, safety, and less likely to cause cerebral edema, hypoglycemia, hypokalemia, and so on. The theoretical basis of small-dose insulin therapy is:
(1) This dose inhibits lipolysis and gluconeogenesis.
(2) This dose is not sufficient to cause potassium translocation into the cell.
(3) Hypoglycemic reactions are almost avoidable.
Specific method of using small-dose insulin: Calculated according to 0.1U/(h-kg), 4-6U per hour is a reliable dose, or it can be injected once an hour or injected intramuscularly once an hour, but the uniform drip is the best therapeutic route. During the treatment, blood glucose, urine glucose and urine ketone body characterization should be measured every 1~2h, so that the insulin dosage can be adjusted according to the measured indexes. According to domestic and international experience, it is generally appropriate to reduce blood glucose by 3.3-3.9mmol/L per hour. It takes about 5-7h from the beginning of the treatment to the blood glucose drop to 13.89mmol/L. The amount of insulin used is usually not more than 50U. If the blood glucose does not drop definitely in 2h after the treatment, the dose of insulin can be doubled. When the blood glucose drops to 13.89mmol/L, 5% glucose solution can be used with insulin (1U of insulin for every 3~5g of glucose, G:R=3:1~5:1) to continue the drip until the urine ketone body disappears. After the patient can enter fluid diet, change to regular subcutaneous injection of insulin.
(c) Potassium supplementation 33% of DKA patients have high blood potassium before the start of treatment, due to the transfer of potassium ions from intracellular to extracellular in acidosis. After treatment, hypokalemia occurs due to hemodilution, restoration of cell volume, correction of acidosis, and restoration of urine flow. If the patient does not have renal insufficiency or anuria, it is usually experienced to administer potassium intravenously as soon as the insulin drip is started and the patient is urinating. The amount of potassium supplementation should not exceed 1.5 g per hour, and the total amount of potassium chloride supplementation should be 6-10 g in 24 h. Reference should be made to the urine volume, blood potassium, or electrocardiogram to guide the amount and rate of potassium supplementation. If the patient is conscious, potassium salt can be taken orally at the same time. If the blood potassium is still low after 2-3d of potassium supplementation, the possibility of magnesium deficiency should be considered, and magnesium supplementation should be tried, and 30% magnesium sulfate can be given as 2.5-5ml intramuscular injection. At present, it is emphasized that patients still need to take 3~4g/d of potassium chloride orally after eating for about one week.
(Correcting acidosis The basis of DKA is the accumulation of ketone bodies, not excessive loss of bicarbonate, and acidosis should not be corrected too early or too quickly. Mild, moderate acidosis, after insulin, ketone body production will stop, the original accumulation of ketone bodies to participate in the tricarboxylic acid cycle oxidation to produce bicarbonate, acidosis can be disappeared by itself.
Acidosis impairs cardiac function, promotes hyperkalemia, and depletes erythrocyte 2,3-diphosphoglycerate, impairing the supply of oxygen to peripheral tissues. However, alkaline supplementation decreases the loss of urea nitrogen, delays the return of blood lactate and ketone body concentrations to normal, and may even stimulate their production. In rat liver perfusion experiments, sodium bicarbonate administration was found to increase acetoacetate. Sodium bicarbonate administration also induced edema formation due to sodium loading. For these reasons, alkalosis should be treated only in severe acidosis, e.g., pH >7.1 or CO2CP <8.9 mmol/L. Sodium bicarbonate should be used instead of sodium lactate. Generally, 125 ml of 5% sodium bicarbonate solution should be given first, and it is better to add water for injection to make isotonic solution (1.25%) before infusion to reduce the incidence of cerebral edema. If blood pH>7.2 or CO2CP≥13mmol/L, stop supplementing alkali.
(v) Phosphate therapy Decrease in blood phosphate concentration due to the introduction of phosphate into insulin-dependent cells as a result of insulin therapy Decrease in 2,3-diphosphoglycerate concentration in DKA Phosphate therapy increases the concentration of 2,3-diphosphoglycerate in erythrocytes to normal. Phosphate therapy increases 2,3-diphosphoglycerate concentrations in erythrocytes to normal. However, there is no benefit of phosphate therapy in DKA. The use of potassium phosphate as a phosphate treatment is inappropriate because potassium and phosphorus have different requirements and can cause abnormal potassium and phosphorus concentrations. Excessive phosphorus supplementation may cause hypocalcemia. Therefore, most authors believe that in DKA, phosphorus should be given only when significant hypophosphatemia occurs.
(f) Treatment of triggers and complications, such as anti-infection, anti-shock, protection of renal function. For the elderly, attention should be paid to thrombosis, especially in the elderly hypertonic state of coma is prone to occur, should be given heparin 5000U, subcutaneous injection every 4 ~ 6h. A rare complication of treatment with a 100% mortality rate is adult respiratory distress syndrome (ARDS), the pathogenesis of which is unknown and may be due to rapid changes in oncotic pressure as a result of intravenous administration of crystalloid solutions, or to acid poisoning and hyperventilation that impairs the permeability of alveolar capillaries. The majority of these patients are those who have had their blood volume corrected with hypotonic solutions.
(VII) Ketone body rebound phenomenon After correction of DKA, some patients showed ketone body rebound phenomenon in the morning of the next day, because it takes a period of time to restore the normal metabolic pathway, we use short-acting insulin 6~12U before bedtime, subcutaneous injection, and add a small amount of food, which can make the ketone body no longer appear in the early morning.
(viii) Resumption of diabetic therapy After DKA is corrected, the original diabetic therapy should be resumed and medication adjustments should be made.
Diabetic ketoacidosis is a metabolic acidosis that occurs in response to a variety of triggers.
Diabetic ketoacidosis refers to diabetic patients in the role of a variety of triggers, such as insulin is significantly insufficient, glucagon inappropriately elevated caused by hyperglycemia, high blood ketones, ketonuria, dehydration, electrolyte disorders, metabolic acidosis and other pathological changes in the syndrome, is one of the emergencies of internal medicine can be a life-threatening. It often occurs in patients with type 1 diabetes. However, diabetic ketoacidosis can also occur in patients with type 2 diabetes.
This question and answer are from the site users, does not represent the position of the site, such as infringement, please contact the administrator to delete.